Beyond the Checklist: A Scaffolded, Experiential Learning Framework for Medical Rescue Simulation (Part 1 of 2)
The effective training of Technical Rescue Specialists (TRS) for high-stakes dynamic environments requires a sophisticated pedagogical approach. This article introduces a comprehensive framework for Simulation-based Education (SBE) designed to elevate Medical Rescue Simulation (MRS). The framework is built upon four interconnected pillars: Foundational Learning Theory, Systematic Skill Scaffolding, Integrated Physical Preparedness, and Stringent Safety Protocols. This article will concentrate specifically on Kolb's learning cycles and the principles of scaffolding. Grounded in Kolb's Experiential Learning Cycle, the framework ensures that learning moves beyond rote memorisation to foster deep understanding and adaptive expertise. The core pedagogical strategy involves scaffolding complex medical rescue procedures, by deconstructing them into isolated, manageable skills. Students’ progress through scenarios of increasing fidelity and complexity, from low-fidelity drills and Visually Enhanced Mental Rescue Simulations (VEMRS) to immersive, high-fidelity exercises, that mirror real-world pressures. This structured progression manages cognitive load, and is designed to cultivate the "emergence" of proficient practice by ensuring foundational competencies are robustly established, thereby preventing the "absence" of critical skills in high-stakes situations.
Introduction
The effective training of Technical Rescue Specialists (TRS) within higher education institutions, particularly in the demanding and high-stakes context of medical rescue operations, requires a pedagogically sound and integrated approach. These environments are characterised by dynamic, unpredictable scenarios that demand not only technical proficiency but also rapid decision-making, physical endurance, and cohesive teamwork [1]. In response to these challenges, Simulation-based Education (SBE) has emerged as a cornerstone methodology, offering a controlled yet realistic platform for the development of critical competencies, reflective practice, and performance assessment [2]. Central to the success of SBE in medical rescue training is a framework built upon four interconnected pedagogical pillars: Foundational Learning Theory, Systematic Skill Scaffolding, Integrated Physical Preparedness, and Stringent Safety Protocols.
These pillars collectively support the development of resilient, competent TRS capable of navigating the complexities of real-world emergencies. However, this article focuses specifically on the first two pillars, foundational learning theory and systematic skill scaffolding, as the primary mechanisms for effective learning within Medical Rescue Simulation (MRS). While the importance of physical conditioning and safety protocols is acknowledged, their detailed exploration falls outside the scope of this article.
The theoretical foundation of this framework draws on Kolb’s Experiential Learning Cycle (ELC), which conceptualises learning as a cyclical process involving concrete experience, reflective observation, abstract conceptualisation, and active experimentation [3,4]. This model ensures that learners engage deeply with simulation scenarios, moving beyond passive participation to develop adaptive expertise through structured reflection and iterative practice. Complementing this, is the principle of scaffolding, informed by Vygotsky’s Zone of Proximal Development (ZPD), which provides a systematic approach to managing cognitive load. By deconstructing complex procedures into isolated skills and gradually increasing scenario fidelity and complexity, scaffolding enables learners to acquire competence incrementally, and with appropriate support [12,15].
This article aims to articulate a theoretically grounded and practically applicable framework for SBE in MRS. By focusing on the foundational mechanisms that underpin effective learning, it offers educators and programme developers a structured guide to optimise simulation design and delivery. Ultimately, this approach seeks to foster the emergence of competent practice while mitigating the risk of absence in critical skills, ensuring that TRS are not only prepared to perform effectively but also to adapt and thrive in the unpredictable realities of emergency medical operations.
Guiding Educational Philosophies for Medical Rescue Simulation (MRS)
The effective training of TRS, particularly within the demanding context of South Africa, necessitates a robust pedagogical foundation. Medical rescue operations are characterised by high stakes, dynamic environments, and the critical need for skilled individuals to work within teams [1]. Simulation-based training has emerged as a cornerstone for developing the requisite competencies, offering a safe and controlled environment for practice and assessment [2].
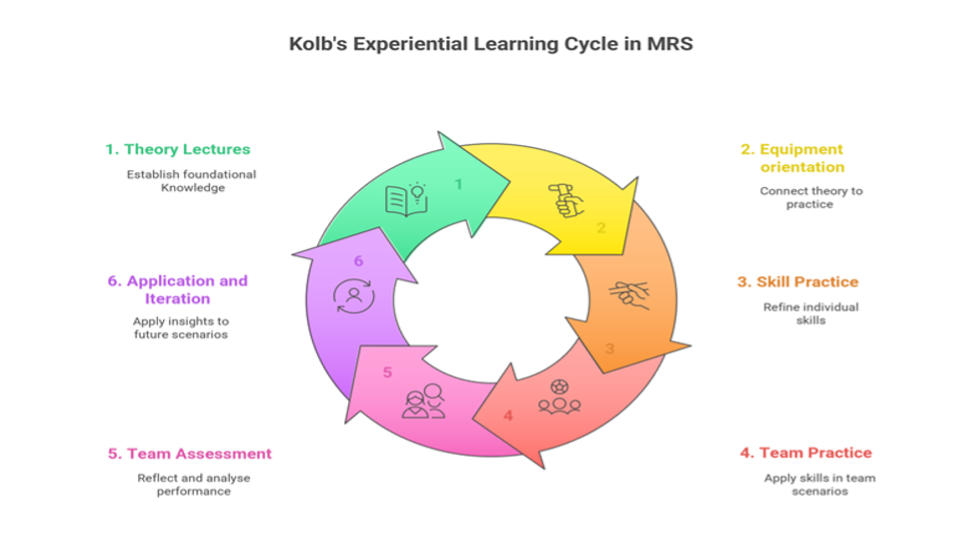
Central to effective MRS is the principle of experiential learning, best exemplified by David Kolb's ELC [3]. This model posits that learning is a cyclical process involving four distinct stages: Concrete Experience (CE), Reflective Observation (RO), Abstract Conceptualisation (AC), and Active Experimentation (AE). This cycle provides a comprehensive framework for designing MRS sequences, that move beyond rote memorisation to foster deep understanding, critical reflection, and adaptive expertise [4].
The integration of Kolb's ELC into a structured MRS curriculum is illustrated below (Figure 2).
● AC - Theory Lectures: The learning journey commences with the introduction of foundational knowledge. During theory lectures, students are exposed to the core concepts, principles, operational protocols, and theoretical underpinnings essential for medical rescue operations. This stage is vital as it establishes the cognitive architecture upon which practical skills and experiential understanding will be built. Without this initial framework, subsequent hands-on activities may lack the necessary context and depth, hindering the development of true comprehension. This aligns with the broader imperative for evidence-based practice in medical rescue, where actions are informed by established knowledge [5].
● CE & AC - Equipment Orientation: This phase serves as a crucial bridge between theoretical knowledge and its tangible application. Students engage in an initial Concrete Experience by physically handling and familiarising themselves with medical rescue equipment. Simultaneously, this interaction reinforces Abstract Conceptualisation, by allowing students to connect the theoretical functions and principles of the equipment (learned in lectures) to its actual features, operation, and limitations. This transitional stage is significant because it embodies the understanding that knowledge must not only be intellectually grasped but also practically engaged with to become meaningful [6].
● CE & RO - Isolated Skills Practice and Sign-off: This stage places a strong emphasis on Concrete Experience through the active practice of specific, discrete medical rescue skills. Students repeatedly perform these skills in a controlled setting. The "sign-off" component, which involves assessment and feedback from instructors, directly facilitates Reflective Observation. Students are prompted to reflect on their performance of each skill, identify areas requiring improvement, and consider the effectiveness of their techniques. This reflection can lead to a refined understanding (AC) of how to execute the skill proficiently. This stage underscores the value of deliberate practice and the indispensable role of structured reflection and feedback in skill acquisition and refinement, linking directly to professional accountability and standards of competence [6].
● CE - Team MRS Practice: Following the mastery of isolated skills, students progress to a more complex and richer experience. Here, they must apply their theoretical knowledge, equipment handling abilities, and individual procedural skills, within a dynamic, interactive, and often immersive team environment. These MRS are designed to mirror the complexities and pressures of real-world medical rescue scenarios. This stage represents the core of experiential learning for professions that rely heavily on teamwork. It shifts the focus from individual skill execution to integrated team performance, fostering an understanding of team dynamics, communication, and coordinated action elements, crucial for successful medical rescue outcomes [7].
The immersive nature of these MRS promotes situated cognition, where learning is deeply embedded in the context of practice [8].
● RO & AC - Team Assessment: This critical stage is heavily weighted towards Reflective Observation and the subsequent development of new Abstract Conceptualisations. Through comprehensive debriefing sessions, performance reviews, and multi-source feedback (including self-assessment, peer feedback, and instructor evaluations), students and teams meticulously analyse what occurred during the MRS. They explore the rationale behind actions taken, the consequences of those actions, and how their collective performance aligned with established principles, protocols, and objectives. This structured reflection is not merely a feedback mechanism; it is a profound learning process that facilitates the deconstruction of the experience, an understanding of cause-and-effect relationships, and the re-conceptualisation of their mental models and approaches [9]. This leads to new insights, modified strategies, and a deeper, more nuanced understanding (AC) of medical rescue operations.
● AE - Application and Iteration: The cycle culminates in Active Experimentation. Based on the rich RO and refined AC generated during the team assessment and debriefing, students plan how to apply their revised understandings and newly acquired insights in future contexts. This could involve subsequent, more challenging MRS, further targeted practice, or, ultimately, application in real-world medical rescue situations, which becomes a new Concrete Experience, restarting the cycle, ideally at a progressively higher level of competence. This stage emphasises that learning is not a terminal event but a continuous, recurring process of action, reflection, and adaptation. This iterative nature is fundamental for professions like medical rescue that demand lifelong learning, continuous quality improvement, and the constant pursuit of enhanced performance [10].
The consistent application of Kolb's ELC in MRS naturally fosters a pedagogical shift from a predominantly didactic, teacher-centred approach, to a more facilitative, student-centred philosophy. The emphasis on students actively engaging in experiences (CE) and critically reflecting on those experiences (RO) empowers them to construct their own understanding and meaning.
Scaffolding the Complex Medical Rescue Procedures Through MRS
The development of proficient and adaptable TRS necessitates pedagogical approaches, that can effectively bridge the gap between theoretical knowledge and the complex, often chaotic, realities of emergency situations [11]. SBE has emerged as a cornerstone in this endeavour, providing a safe yet realistic environment for students to practice and refine critical skills. Within SBE, the principle of scaffolding offers a robust framework for structuring learning experiences, enabling the incremental acquisition of complex medical rescue competencies [15].
The Principle of Scaffolding in SBE
Scaffolding, in an educational context, refers to a process whereby students are provided with temporary, tailored support to achieve learning outcomes that would otherwise be beyond their unassisted reach. This support is gradually withdrawn as the student's proficiency and independence increase [15]. The concept, most famously associated with Vygotsky's (1978) notion of the Zone of Proximal Development (ZPD), posits that learning is most effective when it occurs in the space between what a student can do independently and what they can achieve with guidance [12, 13].
In SBE for complex medical rescue procedures, scaffolding is not merely about simplifying tasks, but about structuring the learning environment to make complex cognitive and psychomotor processes accessible. Medical rescue operations are characterised by high stakes, significant time pressures, dynamic environments, and the need for sophisticated team coordination. These elements can generate considerable cognitive load, potentially overwhelming novice students, and hindering the development of robust skills [14].
A scaffolded approach systematically manages this load, allowing students to focus on specific aspects of performance at different stages of their development [15]. Effective scaffolding aims to reveal the underlying causal mechanisms that constitute competent performance [16]. By providing structured support, instructors can help students identify, understand, and internalise these mechanisms, such as critical decision-making heuristics, effective communication strategies, or precise motor skills, rather than merely mimicking superficial actions [17]. The "emergence" of expert performance is thus cultivated through a carefully modulated process that respects the student's current capacities while strategically expanding them [18].
Breaking Down Procedures: Practising Isolated Skills
Many complex medical rescue procedures are, in reality, a concatenation of several discrete skills and decision points. Attempting to teach or practice such multifaceted procedures, holistically from the outset, can be counterproductive.
The principle of "part-task training," a core element of scaffolding, involves deconstructing a complex skill into its constituent components, allowing students to practice and achieve mastery of these isolated elements before integrating them into a more fluid and comprehensive performance [6].
Figure 3. offers a broad perspective of a high-angle rescue scenario, highlighting the diverse competencies, that rescue students are expected to develop. These constructs, when merged, will showcase, although simplistic and generalised, the activities that will take place during such a medical rescue operation.
Fidelity Progression
Low-fidelity Environment: These may involve basic rope work, like knot making or tabletop exercises. The focus is on fundamental concepts, decision-making processes, and basic procedural steps, without the distraction of highly realistic but potentially overwhelming environmental cues. For example, practising communication protocols or anchor point identification, knot making, etc. To address the multifaceted demands of modern medical rescue incidents, we developed the Visually Enhanced Mental Rescue Simulation (VEMRS) as demonstrated in Figure 4. This low-cost, highly interactive modality is an adaptation of the Visual Enhanced Mental Simulation (VEMS) methodology created for training in resource-constrained environments [19]. VEMRS deliberately shifts the focus from singular patient care to the wider operational landscape, challenging students with issues of incident command, inter-agency communication, and strategic decision-making under pressure [20]. Adopting VEMRS functions as more than a training tool; it is a research platform for identifying the deep-seated causal mechanisms, like team dynamics and communication habits, that are pivotal in determining medical rescue outcomes [21].
Medium-fidelity Environment: These might incorporate controlled outdoor training sites capable of exhibiting physiological responses, more realistic equipment, and some environmental distractors. Students begin to integrate skills in a more contextualised manner.
High-fidelity Environment: These are designed to closely mirror the complex and unpredictable nature of real-world situations. By incorporating authentic locations, such as mountainous terrain, these environments introduce genuine uncertainty and time pressures, requiring participants to quickly adapt. The involvement of live actor patients further increases the realism, compelling participants to integrate all necessary skills while under significant stress.
The pursuit of authenticity, however, increases the risk of physical injury. The dynamic and uncontrolled elements present in such environments, require strong safety measures. To mitigate these risks, it is essential to conduct comprehensive risk assessments, hold mandatory safety briefings, ensure the presence of dedicated safety officers with clear authority to intervene, and establish emergency protocols. These measures are vital to guarantee that the valuable and immersive learning experience does not compromise students' well-being, balancing realism with strict safety oversight.
Complexity Progression
Complexity can be increased by manipulating variables such as:
Number of Tasks: Starting with single-focus scenarios, and moving towards multi-tasking requirements.
Information Load: Initially providing clear and unambiguous information, then introducing incomplete or conflicting data.
Environmental Stressors: Adding background noise, weather, or challenging physical spaces.
Team Dynamics: Progressing from individual tasks to scenarios requiring intricate interprofessional collaboration and communication.
Patient Condition: Starting with stable patients or single pathologies and advancing to deteriorating patients with multiple co-morbidities.
This progressive approach ensures that students are continually challenged but not excessively overwhelmed. Each stage builds upon the last, allowing for the consolidation of learning and the gradual development of resilience and adaptability. From a critical realist standpoint, the increasing complexity and fidelity seen in Figure 5. allow for the interaction of more numerous and varied causal mechanisms, providing students with insight into how these mechanisms interplay in real-world settings to produce outcomes [22]. The "geo-history" of the student, their prior experiences and learning trajectories, also informs their engagement with these progressively complex scenarios, highlighting the individualised nature of skill emergence [23].
Principles of Scaffolding in High-Angle Medical Rescue Training
In SBE, the concepts of fidelity and complexity progression are closely intertwined. For example, when applying scaffolding principles in high-angle rescue training, students progress from scenarios with low complexity and high levels of support to those with greater complexity and reduced support. Throughout this progression, the level of instruction, hands-on practice, and feedback is gradually adjusted to match the student’s development and needs [24].
Basic Knot Tying and Equipment Familiarisation
Low Complexity, High Support:
● Instruction: Direct, step-by-step demonstration of each knot (e.g., figure-eight, double fisherman's) and explanation of each equipment piece (e.g., carabiners, belay devices, ascenders).
● Practice: Repetitive, isolated practice of individual knots on a rope segment or familiarisation with equipment function in a low-pressure setting.
● Feedback: Immediate, prescriptive correction and verification of accuracy by the instructor.
Set Up of a Single Person Ascend and Descend Line
Medium Complexity, Medium Support:
● Instruction: Guided demonstration of how to integrate known knots and equipment (harness, descender/ascender, belay device, anchor) for personal ascent/descent.
● Practice: Supervised students practice on a low, stable structure (e.g., a training tower or short wall) with redundant safety systems in place.
● Feedback: Real-time coaching on body mechanics, safety checks, and procedural flow; interventions for significant errors.
Set Up of a Basic Mechanical Advantage System
Medium Complexity, Medium Support:
● Instruction: Explanation of principles of mechanical advantage (e.g., 3:1, 5:1 systems) and demonstration of combining rope, pulleys/carabiners, and anchors to build a simple system.
● Practice: Team-based exercises to assemble and operate the system with a non-critical load (e.g., a rescue dummy) on flat ground or a gentle slope.
● Feedback: Focus on correct rigging, load management, and team communication; troubleshooting common issues as they arise.
Apply Medical Rescue Techniques to Different and Novel Environments
High Complexity, Low Support:
● Instruction: Scenario-based briefings with minimal direct instruction on specific techniques; emphasis on problem-solving and adaptation.
● Practice: Full-scale exercises in varied, less predictable environments (e.g., multi-story structures, natural rock faces, confined spaces) with complex scenarios and potential stressors (e.g., noise, limited visibility).
● Feedback: Instructor primarily observes, intervenes only for critical safety concerns, and facilitates comprehensive debriefings focused on decision-making, risk assessment, team coordination, and adaptive problem-solving under pressure. Students are encouraged to self-assess and provide peer feedback.
This allows students to develop the specific motor skills and cognitive understanding required for each step without the immediate pressure of managing the entire scenario. Once proficiency in these isolated skills is demonstrated, they can be progressively chained together. This methodical approach ensures that foundational competencies are robustly established, which is critical for the successful "emergence" of the more complex, integrated skill. The "absence" of a specific foundational skill can lead to cascading failures in a real-world medical rescue operation; isolated practice helps identify and remediate such potential absences early in the MRS process. This aligns with a critical realist emphasis on understanding how component parts (mechanisms) contribute to the functioning (or dysfunctioning) of the whole system [25].
Progressive Scenario Design: From Low to High Fidelity and Complexity
Effective scaffolding in SBE extends beyond individual skills to the overall design of MRS scenarios. Progressive scenario design involves a deliberate and incremental increase in both the fidelity and complexity of MRS as students advance [26].
Techniques for Effective Scaffolding (Micro-level)
Beyond the macro-level design of curricula and scenarios, effective scaffolding relies on specific techniques employed by instructors during the MRS and debriefing phases. These micro-level interactions provide crucial real-time support and guidance [27].
Clear Pre-briefing: Before a scenario begins, instructors must clearly articulate the learning objectives, the expected level of performance, the available resources, and the degree of support that will be offered. This manages student expectations and focuses their attention [28].
Thinking Aloud: Encouraging students to verbalise their thought processes during a scenario can provide instructors with insights into their decision-making and allow for timely, targeted guidance. It also helps students to self-monitor and reflect-in-action [29].
Prompting and Cueing: When students encounter difficulties, instructors can provide subtle hints, questions, or direct cues to guide them towards appropriate actions or considerations. This might involve drawing attention to a critical piece of data or suggesting a potential intervention. The level of prompting should be inversely proportional to the student's developing expertise [30].
Structured Feedback: Providing specific, objective, and constructive feedback, both during (if appropriate and aligned with the scaffolding strategy) and after the scenario, is essential. This feedback should focus on observed behaviours and their consequences, linking them to the underlying principles and mechanisms of effective care [31, 32].
Pause and Discuss: In some instances, particularly during formative learning, it can be beneficial to temporarily pause the MRS to discuss a critical decision point, clarify a misunderstanding, or reinforce a teaching point before resuming the scenario [33].
Gradual Withdrawal of Support (Fading): As students demonstrate increased competence and confidence, the instructor systematically reduces the level of prompting, cueing, and direct intervention. This encourages greater autonomy and allows students to take fuller ownership of the problem-solving process [30].
Effective Debriefing: The post-scenario debriefing is a cornerstone of SBE and a critical component of scaffolding. Instructors should guide a reflective discussion that encourages students to explore not only what happened, but why it happened and how it could be improved. This involves examining the causal chains of events, the decisions made (and their rationales), and the impact of team interactions [34]. An informed debriefing might explicitly probe the interplay of contextual factors, individual actions, and underlying mechanisms that shaped the scenario's outcomes [35]. These micro-level techniques, when skilfully applied, create a dynamic and responsive learning environment that supports students in navigating complex challenges and internalising the deep structures of proficient medical rescue practice [27].
Scaffolding complex medical rescue procedures through SBE is a powerful pedagogical strategy that aligns with the demands of preparing TRS for high-stakes environments. By systematically breaking down procedures, progressively designing scenarios from low to high fidelity and complexity, and employing effective micro-level support techniques, instructors can create pathways for students to develop the robust, adaptable competencies required in medical rescue. This approach not only fosters the emergence of proficient performance but also cultivates a deeper understanding of the causal mechanisms that underpin successful outcomes in medical rescue situations. Such a structured, yet adaptable, pedagogical framework is indispensable for programmes aiming to produce critically thinking and highly capable TRS.
Conclusion
The systematic scaffolding of complex medical rescue procedures, through deliberate progression in simulation fidelity and task complexity, alongside the decomposition of procedures into discrete, manageable skills, effectively mitigates cognitive and psychomotor overload. This structured approach facilitates the incremental development of proficiency, enabling learners to build upon foundational competencies in a manner that supports the emergence of expert performance.
While the broader framework of MRS encompasses four interconnected pillars, this article has primarily focused on the pedagogical dimensions of foundational learning theory, and systematic skill scaffolding as critical drivers of effective SBE. The remaining pillars, which are integrated physical preparedness and stringent safety protocols, although acknowledged as essential to the holistic development of TRS, were not the central focus of this article. Their roles in ensuring physical readiness and safeguarding psychological and physical well-being warrant dedicated exploration in future work.
By emphasising the theoretical and instructional foundations of simulation, this article contributes to the advancement of evidence-informed practices in medical rescue training. Institutions committed to producing competent, resilient, and critically thinking TRS must adopt such structured and theory-driven approaches to SBE, ensuring that learners are equipped not only with technical expertise, but also with the cognitive agility required to navigate the complexities of real-world emergencies.
Author contributions
All authors contributed equally and validated the final version of record.
Declarations
Conflicts Of Interests
The Authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Registration
No registration applicable.
Data availability statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Ethical approval
Ethical approval for this study was not required.
References
1. Hooshangi N, Mahdizadeh Gharakhanlou N, Ghaffari-Razin SR. Urban search and rescue (USAR) simulation in earthquake environments using queuing theory: estimating the appropriate number of rescue teams. Int J Disaster Resil Built Environ. 2024;15(1):1‒18. https://doi.org/10.1108/IJDRBE-09-2021-0122
2. Elendu C, Amaechi DC, Okatta AU, Amaechi EC, Elendu TC, Ezeh CP, et al. The impact of simulation-based training in medical education: a review. Medicine (Baltimore). 2024;103(27):e38813. https://doi.org/10.1097/MD.0000000000038813
3. Secheresse T, Pansu P, Lima L. The impact of full-scale simulation training based on Kolb’s learning cycle on medical prehospital emergency teams: a multilevel assessment study. Simul Healthc. 2020;15(5):335‒340. https://doi.org/10.1097/SIH.0000000000000461
4. Wijnen-Meijer M, Brandhuber T, Schneider A, Berberat PO. Implementing Kolb’s experiential learning cycle by linking real experience, case-based discussion and simulation. J Med Educ Curric Dev. 2022;9:23821205221091510. https://doi.org/10.1177/23821205221091511
5. Smith M. Experiential learning experiences of emergency medical care students at a selected University in KwaZulu-Natal [Dissertation for the Degree of Master of Health Sciences]. [Durban, South Africa]: Durban University of Technology; 2018. https://doi.org/10.51415/10321/3093
6. Taraporewalla K. The Adaptation of Motor Learning Theory in Medical Procedural Tasks [PhD Thesis]. Faculty of Medicine, The University of Queensland; 2024. https://doi.org/10.14264/ea20136
7. Zawawi AA, Halim NA, Kamarunzaman NZ, Zawawi AA, Halim FW. The linkage between team communication, team motivation and search and rescue team performance. SA J Hum Resour Manag. 2023;21:10. https://doi.org/10.4102/sajhrm.v21i0.2217
8. Chernikova O, Heitzmann N, Stadler M, Holzberger D, Seidel T, Fischer F. Simulation-based learning in higher education: a meta-analysis. Rev Educ Res. 2020;90(4):499‒541. https://doi.org/10.3102/0034654320933544
9. Chan CKY, Lee KKW. Reflection literacy: a multilevel perspective on the challenges of using reflections in higher education through a comprehensive literature review. Educ Res Rev. 2021;32:100376. https://doi.org/10.1016/j.edurev.2020.100376
10. Abdullah N, Rose J, Brown E, Geduld H. Vehicle extrication in road traffic crashes: a descriptive analysis of an advanced medical rescue service in South Africa. Afr J Emerg Med. 2025;15(2):621‒7. https://doi.org/10.1016/j.afjem.2025.04.003
11. Altmiller G, Pepe LH. Influence of technology in supporting quality and safety in nursing education. Nurs Clin North Am. 2022;57(4):551‒62. https://doi.org/10.1016/j.cnur.2022.06.005
12. Shabani K, Khatib M, Ebadi S. Vygotsky’s zone of proximal development: instructional implications and teachers’ professional development. English Lang Teach. 2010;3(4):237. https://doi.org/10.5539/elt.v3n4p237
13. Sellberg C, Mona L, Saljo R. Assessment in the zone of proximal development: simulator-based competence tests and the dynamic evaluation of knowledge-in-action. Classroom Discourse. 2022;13(4):365‒85. https://doi.org/10.1080/19463014.2021.1981957
14. Esmaeili R, Yazdi M, Rismanchian M, Shakerian M. Unveiling the dynamics of team cognition in emergency response teams. Front Psychol. 2025;16:1534224. https://doi.org/10.3389/fpsyg.2025.1534224
15. Masava B, Nyoni CN, Botma Y. Scaffolding in health sciences education programmes: an integrative review. Med Sci Educ. 2023;33(1):255‒73. https://doi.org/10.1007/s40670-022-01691-x
16. Stutchbury K. Critical realism: an explanatory framework for smallscale qualitative studies or an ‘unhelpful edifice’? Int J Res Method Educ. 2022;45(2):113‒28. https://doi.org/10.1080/1743727X.2021.1966623
17. Thornhill-Miller B, Camarda A, Mercier M, Burkhardt J-M, Morisseau T, Bourgeois-Bougrine S, et al. Creativity, critical thinking, communication, and collaboration: assessment, certification, and promotion of 21st century skills for the future of work and education. J Intell. 2023;11(3):54. https://doi.org/10.3390/jintelligence11030054
18. Sobuwa S. A critical realist study into the emergence and absence of academic success among Bachelor of Emergency Medical Care students [Doctoral Thesis]. University of Cape Town; 2018. Available from: http://hdl.handle.net/11427/29475
19. Alinier G, Meyer J, Naidoo V, Campbell C. Simplifying simulated practice for healthcare professionals and educators. J Emerg Med Trauma Acute Care. 2016;2016(2):1. https://doi.org/10.5339/jemtac.2016.icepq.79
20. Dogan B, Pattison N, Alinier G. A form of mental simulation with significant enhancements enabling teamwork training. Int J Healthc Simul. 2021;1(1):56‒60. https://doi.org/10.54531/JSHC9951.
21. Brazil V, Speirs C, Scott C, Schweitzer J, Purdy E. Recommendations for the design and delivery of visually enhanced mental simulation: insights from participants and facilitators. J Healthc Simul. 2025;1‒11. https://doi.org/10.54531/NDXV6633
22. Swart R, Duys R, Hauser ND. SASS: South African Simulation Survey ‒ a review of simulation-based education. S Afr J Anaesth Analg. 2019;25(4):12‒20.
23. Khalid AF, George MA, Eggen C, Sritharan A, Wali F, Viens AM. Using Simulation-Based Experiential Learning to Increase Students’ Ability to Analyze Increasingly Complex Global Health Challenges: A Mixed Methods Study. medRxiv. 2023 Jan 1;2023.12.19.23300262. https://doi.org/10.1101/2023.12.19.23300262
24. Bauer E, Heitzmann N, Fischer F. Simulation-based learning in higher education and professional training: approximations of practice through representational scaffolding. Stud Educ Eval. 2022;75:101213. https://doi.org/10.1016/J.STUEDUC.2022.101213
25. Owen JR, Kemp D, van der Watt P, Harris J, Li Ern Ang M, Marais L. Disaster scenes as a foundation for emergency response planning. Int J Disaster Risk Reduct. 2024;113:104795. https://doi.org/10.1016/j.ijdrr.2024.104795
26. Fraser KL, Ayres P, Sweller J. Cognitive load theory for the design of medical simulations. Simul Healthc. 2015;10(5):295. https://doi.org/10.1097/SIH.0000000000000097
27. Masava B, Nyoni CN, Botma Y. Standards for scaffolding in health sciences programmes: a Delphi consensus study. J Med Educ Curric Dev. 2023;10:23821205231184045. https://doi.org/10.1177/23821205231184045
28. Hughes PG, Hughes KE. Briefing prior to simulation activity. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025. Available from: https://www.ncbi.nlm.nih.gov/pubmed/31424818
29. Abdulmohdi N, McVicar A. Investigating the clinical decision-making of nursing students using high-fidelity simulation, observation and think aloud: a mixed methods research study. J Adv Nurs. 2023;79(2):811‒24. https://doi.org/10.1111/JAN.15507
30. Poledna M, Gomez-Morales A, Hagler D. Nursing students’ cue recognition in educational simulation: a scoping review. Nurse Educ. 2022;47(5):283‒7. https://doi.org/10.1097/NNE.0000000000001198
31. Ludeke AK, Olaya JFG. Effective feedback, an essential component of all stages in medical education. Universitas Medica. 2020;61(3):1‒15. https://doi.org/10.11144/Javeriana.umed61-3.feed
32. Ajjawi R, Bearman M, Molloy E, Noble C. The role of feedback in supporting trainees who underperform in clinical environments. Front Med (Lausanne). 2023;10:1121602. https://doi.org/10.3389/fmed.2023.1121602
33. Lee JY, Szulewski A, Young JQ, Donkers J, Jarodzka H, van Merrienboer JJG. The medical pause: importance, processes and training. Med Educ. 2021;55(10):1152‒60. https://doi.org/10.1111/medu.14529
34. Decker S, Alinier G, Crawford SB, Gordon RM, Jenkins D, Wilson C. Healthcare Simulation Standards of Best Practice™: the debriefing process. Clin Simul Nurs. 2021;58:27‒32. https://doi.org/10.1016/j.ecns.2021.08.011
35. Abulebda K, Auerbach M, Limaiem F. Debriefing techniques utilized in Medical Simulation. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025. Available from: https://www.ncbi.nlm.nih.gov/pubmed/31536266